QCOSTARICA – In contrast to the belief that only the old get deadly sick after being infected with covid-19, a 27-year-old old and a healthy man before SARS-CoV-2 has accumulated so far 111 days connected to a device popularly known as an “artificial lung”.

Technically, it is ECMO, or extracorporeal membrane oxygenation therapy, a machine that temporarily replaces their damaged lungs as they try to recover from the injuries caused by COVID-19.
The young man, who had neither diabetes, obesity, or hypertension, is one of the 11 patients currently receiving ECMO in one of the Intensive Care Units (ICU) of the Calderón Guardia Hospital.
The exponential surge in cases meant that all available equipment is assigned to a Covid-19 patient in critical condition.
“He is no longer covid. The covid comes, causes damage and leaves. (The virus) left sequelae of fibrosis or inflammation, which is what we are seeing now: super-aggregated infections (sic) by hospital germs.
“It is what has had that patient so many days with infection after infection, effusions in the pleura, in the pericardium. It has been a snowball, that the covid came, pushed it, and left. It threw the stone and hid its hand,” explained Dr. Jorge Arturo Ramírez Arce, ECMO coordinator and specialist in Intensive Care at Calderón Guardia.
Costa Rica is the only country in Central America that offers a consolidated program of ECMO therapy. With the pandemic, 31 very seriously ill patients from covid-19 have benefited since August 2020, including the 11 who are currently on that therapy.
If at any given moment the resource is only enough to see five severe patients instead of one critical one, I will have to dedicate myself to seeing the severe ones because they have a better chance of surviving than the critical one.Dr. Jorge Arturo Ramírez Arce, ECMO coordinator and specialist in Intensive Care at Calderón Guardia
The program began to take shape in 2012, with the training of personnel and the purchase of equipment, but it is consolidated two years later. The Caja Costarricense de Seguro Social (CCSS) grants Calderón Guardia the title of ECMO National Reference Center.
Together with Jorge Arturo Ramírez Arce there is a team of specialists in Critical Care, Nursing, Pulmonology, Cardiology, Peripheral Vascular and Psychology, to mention just some of the areas that intervene in the approach to these patients.
ECMO, explains Ramírez – who specialized in Paris, France –, is an extracorporeal life support therapy in which the techniques of circulation and oxygenation of the blood outside the body with the support of devices have been perfected.
Furthermore, it is one of the most sophisticated therapies for Intensive Care patients, which are applied only at the so-called “fourth level of health,” the highest.
“It is no longer used for short periods, as it was done at the beginning with cardiac surgeries, or with a stopped heart. Technology has managed to extrapolate this to Intensive Care beds, placing a similar therapy at the bedside of the patient to make a substitution (of organs),” explained the intensivist.
This therapy can be put into two modalities. The first, as respiratory support, or veno-venous ECMO. The second, as a cardiac support therapy (for heart failure) with pulmonary involvement, or veno-arterial ECMO.
It is not a new therapy, clarifies Ramírez, who has more than 50 years in medicine. “It is not a treatment that cures either, it is a bridge therapy,” he clarified.
“We are experts in saving time replacing organ functions while the patient heals from an infection. ECMO saves time by substituting functions so that this organ recovers,” explained the specialist.
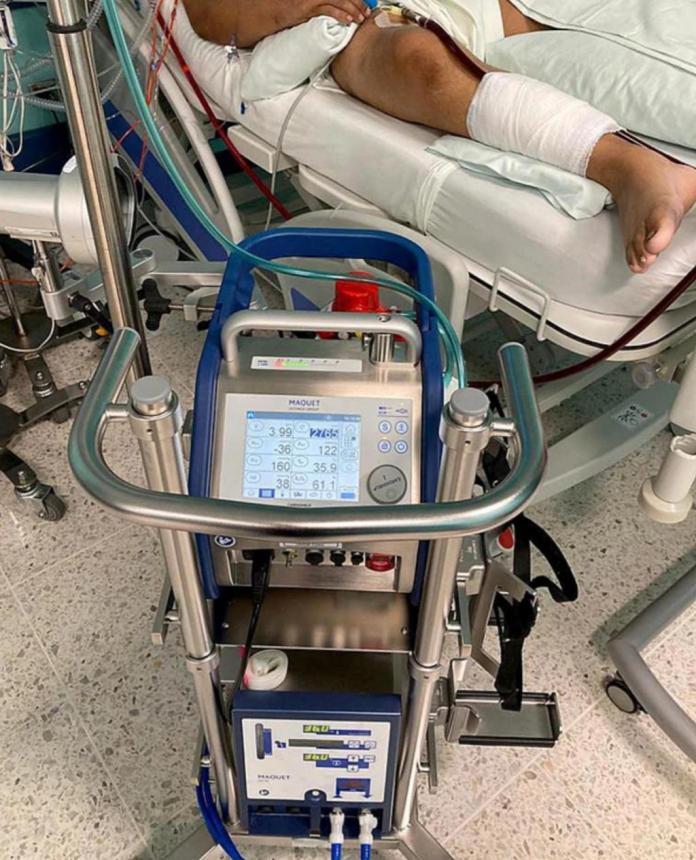
ECMO in pandemic
The extracorporeal oxygenation membrane is also known as “the machine that resuscitates people and organs.”
Before the pandemic, the patients who most required this approach were those with pulmonary edema due to injury, caused, among other things, by inflammation of the lung or, as Ramírez explains, caused by other inflamed organs.
It was common to see this type of case in burn patients, with severe pancreatitis or pneumonia. Also in the Calderón they treated patients from the previous pandemic: 17 affected by AH1N1, an influenza virus.
In total, since 2014 they have treated 161 patients.
“With the advent of covid, it is different. It has been raged with greater severity and mortality, to the point that everyone in the world recognizes that while the patient is running on ECMO, it is no longer two weeks (average time of a non-covid patient connected to ECMO), but a much longer time.
“Of those who have survived, on average it is 45 days of ECMO, when we were used to treating them with this therapy for two weeks. After so long, we are giving more time for infectious complications to appear due to lying down, in an induced coma: the longer the therapy is prolonged, the more chance there is for complications to appear,” explained Ramírez Arce.
These complications are what have kept the 27-year-old in delicate condition. Only in this patient, only in hospital stay in ICU, the CCSS has invested more than ¢220 million colones (US$364,000 dollars) in his care, not counting supplies and treatments such as the extracorporeal oxygenation membrane.
Another man, the second-longest recorded time connected to this membrane, has accumulated 104 days.
Of the 11 connected to this therapy today, only this 27-year-old is out of the norm. The rest are people with various risk factors, including the best known: obesity (with body mass indexes of 44), diabetes, or hypertension.
In the group of patients there are morbidly obese, with weights of up to 150 kilos, reported Ramírez.
This condition makes it difficult to apply the technique, because inserting the cannula (a thin tube inserted into a vein or body cavity) becomes very difficult, explained the intensivist.
Of the 31 patients, 11 are currently in treatment, and nine have already recovered. The other 11 died.
Among those rehabilitated, there are four doctors who were infected while treating patients with covid-19. Two of them have already returned to their work.

At full capacity
Of the total number of covid-19 cases, explains Ramírez, 5% will need an ICU. Of those, 3% will require mechanical ventilation, and of those ventilated, he said, at least one in 15 will need ECMO therapy.
The increase in the number of patients will logically lead to an increase in the demand for this therapy.
“We have had patients who meet criteria and they cannot be supported because we are at full capacity. We are in the task of getting more units. But even if I had 20 ECMOs, I also don’t have what is most important: an ICU is not a bed with a monitor. Attention is not made by machines, monitors or beds, it is done by trained personnel. And this is what is missing right now,” warned the specialist.
The ECMO does not work with waiting lists, clarified the doctor. Although he does not keep a record of this, Ramírez does know of patients who, needing this therapy, did not get it because there is no capacity.
“They are young people who die,” said the doctor. In the Calderón Guardia, he knows of at least five such cases.
“ECMO, which is a life-saving therapy, can be compromised at some point by the (increase in) number of patients. If at any given moment the resource is only enough to see five severe patients instead of one critical one, I will have to dedicate myself to seeing the severe ones because they have a better chance of surviving than the critical one.
“If the health system reaches a point of stress, in which it is not possible to provide the latest quality of care, this type of therapy will not be able to be sustained. Then, it is the moment that even, worldwide, it is considered to stop offering therapy and dedicate oneself to those who have the best chance of survival.
“We are not there yet, but we are very close,” warned Ramírez.
Article was translated and adapted from La Nacion “Paciente de 27 años lleva 111 días conectado a ‘pulmón artificial’ tras infectarse de covid-19”. Read the original article in Spanish here.

